
Type 1 diabetes (T1DM) is an autoimmune condition characterised by the production of antibodies that act against pancreatic beta-cells leading to insulin deficiency and ultimately an absolute need for exogenous insulin to survive.
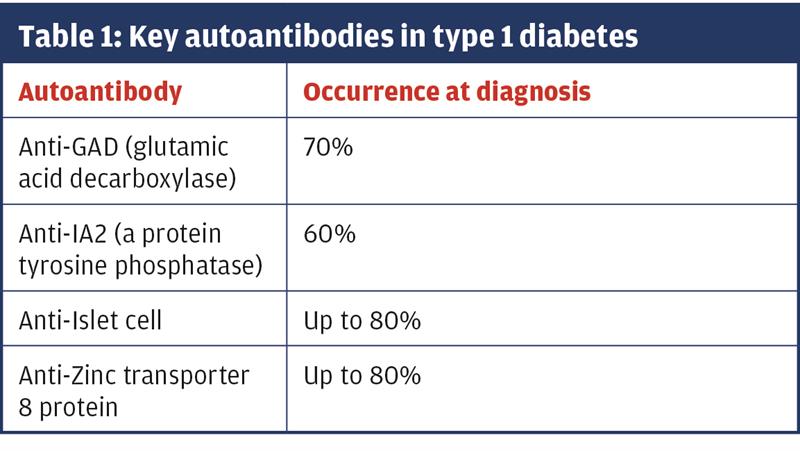
Some of the key antibodies that are commonly used as markers for T1DM are shown in table 1.1 The greater the number of beta-cell antibodies identified the more likely the progression to T1DM. At the point of diagnosing diabetes around 85-90% of cases that are subsequently confirmed as T1DM will test positive for one or more of these autoantibodies.
Looking at genes relevant to the risk of developing T1DM, the most important appear to be those located in the major histocompatibility complex (MHC) on chromosome 6 that can either predispose to or protect against the occurrence of T1DM. Specifically, HLAs (human leucocyte antigens) DQ2, DQ8 and DR3/DR4 are commonly found in T1DM whereas HLA-DQ6 and DR2 exert a protective effect against T1DM.2 In genetically predisposed individuals environmental factors, such as a viral infection, may then trigger the pathway to T1DM.
Register now for access
Thank you for visiting Independent Nurse and reading some of our premium content. To read more, please register today.
Register
Already have an account? Sign in here
