
There were several thousand alcohol-specific deaths in the UK during 2016, new figures from the Office of National Statistics (ONS) have revealed.
Alcohol-specific deaths reached 7,327 in 2016, meaning an age-standardised rate of 11.7 deaths per 100,000 people in the UK. Death rates were also considerably higher for those aged 55 to 64 years of age and for those that lived in the most deprived local areas.
Responding to the figures, Councillor Izzi Seccombe, Chairman of the Local Government Association’s Community Wellbeing Board, said: ‘It is tragic that 7,327 men and women in the UK died because of alcohol last year. Behind these appalling statistics are real people - fathers, mothers, sons, daughters, husbands and wives.
‘Alcohol-related deaths are preventable, and councils would be able to do more if government reverses the cuts to the public health grant in the Autumn Budget.’
In the UK, since 2001, rates of alcohol-related deaths were an average of 55% higher for men than for women. Men aged between 60 and 64 years had a death rate of 40.3 per 100,000, a stark change from 2001 when the age group with the highest rate (34.3) was men aged 55 to 59.
This coincides with an alarming shift in the number of elderly men dying from alcohol-specific deaths since 2001. Between 2001 and 2016 alcohol-specific death rates among men aged 70 to 74 rose by almost 50%.
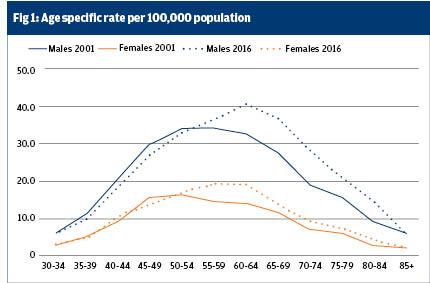
The new figures for 2016, however, revealed that, for both sexes, alcohol-specific deaths were highest for those aged between 55 and 64 years of age. Although these rates remain largely unchanged since 2013, the shift towards older people suffering from alcohol-specific deaths is a concern.
Izzi Seccombe said: ‘What is particularly concerning about these figures is that the rates of alcohol-related deaths were highest in middle aged and older age groups. Despite drinking comparatively little, older people consume alcohol far more often.’
The figures also revealed an uneven geography of deaths, with rates being significantly higher in the most deprived local areas. Scotland had the highest rate of alcohol-specific deaths rates (30.9 out of 100,000) out of the 4 nations, although this was considerably lower than in 2001 when the rate was 39 per 100,000 – a decrease of 21% over the period.
Although the highest, Scotland was the only country to experience a decrease in their alcohol-specific death rates, with England, Wales and Northern Ireland all witnessing a rise since 2001.
In England, and for both sexes, death rates were higher in the North of the country, with the lowest rates being in the East of England for men and in London for women. All regions of England, apart from London, have seen their death rates increase since 2001.
The ONS has said: ‘A possible explanation for regional differences in alcohol-specific deaths could be that those in deprived areas are differentially affected by the alcohol they consume.
‘Specifically, the alcohol consumption harm paradox shows that consumption in more deprived areas can often be the same or even less than that in less deprived areas, but harm is elevated in the more deprived areas.’
Responding to the new findings, Rosanna O’Connor, Director of Drugs, Alcohol and Tobacco at PHE, said: 'Nurses are well placed to identify risky drinking and NICE encourages the use of questionnaires to identify these patients and give support, advice and encouragement or referral onto specialist services, to help reduce their drinking and risk of harm.
'Primary care and community nurses may also work within hospital alcohol care teams to help manage patients with substantial alcohol problems, which will contribute to reducing the burden on the NHS.'
